Wash your hands regularly. This is something we’re all taught from a young age to protect ourselves from sickness caused by exposure to pathogenic microorganisms.
I use the word reduce, because using soap and water does not sterilize your hands. Hand sterility is rarely required outside of a medical setting and using a properly applied alcohol gel is the most common way to achieve it. It’s such an aggressive technique that regular cleaning this way leads to the cracked and bleeding skin that many healthcare professionals experience.
Instead, when we wash our hands with soap and water we are only aiming to reduce the number of bacteria present to safe levels and remove stains, greases, and odors.

The soap element of the hand washing process does far less of the work than you might think. Many studies show similar levels of bacterial reduction when comparing washing with soap and water with just water on its own.
A lesser known fact is that soap might leave your hands dirtier than before you washed. Studies conducted in the USA, Japan, and the UK have revealed that up to 1 in 4 “top-up” or “bulk-fill” dispensers contain excessive levels of bacteria not suitable for the cleaning of hands. The problem is recognized as a health risk by the Center for Disease Control and Prevention (CDC) within healthcare settings.
“Top-up” and “Bulk-fill” dispensers are those that have a bottle or container that is refilled as it runs low. This is most commonly seen in commercial facilities and transportation hubs due to their aesthetically pleasing appearance favored by architects and their flexible approach to soap use which allows facility management teams to drive down consumable costs.
Bacteria are introduced to these products both during the refilling process and during use, as contaminated air is drawn into the container to replace the soap that is dispensed. The containers are warm and wet, ideal breeding grounds for certain microorganisms, which over time form large enough colonies as to become unhealthy. While that might seem unlikely due to the nature of soap, many bacteria can survive in the most unlikely of places, including diesel tanks, alcohol, and even thermal vents under the sea. Some bacteria have even been proven to survive in the vacuum of space. Suddenly it doesn’t seem so strange they might be in our soap.

Once a bacterial colony count reaches a certain size, biofilms can be formed and are identified as a mucus-like substance within the soap. This can block tubes or place strain on pumps, leading to product failure, a common problem with “bulk fill” systems.
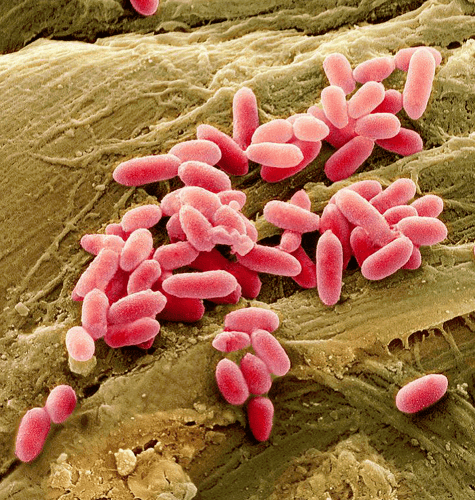
My own personal testing of soap from these types of products has identified colonies of bacteria from several different species, some more nefarious than others including Pseudomonas Aeruginosa, which can cause skin rashes (Often know as hot tub rash). For people who suffer with immune-deficiencies, exposure to these bacteria can result in serious infections, sepsis, or even death.
“Closed systems” are much cleaner. Soap is usually stored in a bag, which is then replaced with a fresh, clean supply as it runs out. However, the cost of the consumable is usually higher than their less clean “bulk-fill” counterparts and architects are very limited in delivering the aesthetic restroom experience they intend to achieve for their clients.
While the phenomenon of bacteria in soap is recognized in healthcare settings, it is not widely discussed within regular facilities management and is very difficult, if not impossible, to trace back to source. How many times have you had a rash or fell ill on vacation and blamed it on the pool, local water, or food? Perhaps it was when you washed your hands at the airport. Perhaps it was in the restroom at the all-inclusive resort.
Because of the lack of traceability, architects and facilities design companies are unlikely to change their habits, but if you’re designing a restroom right now, think carefully before selecting hygiene products for your project. There are soap dispensers that can offer both a clean washing experience and pleasing aesthetics. Ensure the dispenser you choose can be disassembled and maintained, and if possible, features materials resistant to bacteria. Allow for proper maintenance within your room design as well, so facilities teams can easily remove, clean, and sterilize products periodically.
‘It’s not a problem for me, my soap brand kills 99.9% of bacteria’
If this is going through your mind, think again. The 99.9% claim is one of the most misleading claims ever printed on a product. It does not mean it kills the bacteria we are trying to avoid. Many bacteria are completely immune to the levels of biocide used within these soap products. In fact, the aforementioned Pseudomonas Aeruginosa seems completely unaffected by it.
Don’t panic! We’re not all going to become sick from washing our hands, and not all soap dispensers harbor dangerous bacteria. I’m certainly not suggesting people should stop using soap in their day to day lives. It is still recognized as the most effective way to avoid sickness.
In an age where bacteria are becoming immune to certain biocides and antibiotics, we should be conscious of the different ways we encounter them. We should offer people with special health requirements the tools they need to avoid possible exposure and arm cleaning teams with knowledge to further develop good hygiene practices, such as the regular sterilization of soap dispensers.



Enjoy this blog? Leave a comment or ask a question!